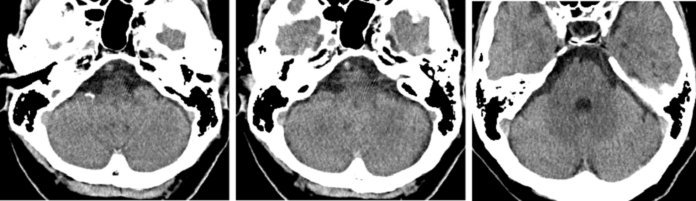
Case study: basilar artery occlusion
Studies have shown that the prognosis of patients with sudden-onset sensorineural hearing loss is good. The hearing loss is generally because of idiopathic sudden deafness, perilymphatic fistula and Meniere’s disease. In some rare cases, it is also because of vertebrobasilar ischemia because of basilar artery occlusion. The incidence of vertebrobasilar ischemia is approximately 1.2% in sudden sensorineural hearing loss.
The anterior-inferior superior artery, originating from the basilar artery (BA), is also known to contribute to acute sensorineural hearing loss. In addition, bilateral deafness because AICA ischemia presents with brainstem signs and symptoms. However, rarely because of a single factor. But in cases where the hearing loss is because of vestibular occlusion, the prognosis is poor.
This article reports the case of a woman who presented with bilateral hearing loss because of vertigo and vomiting. According to the study, initially, it was not suspected that the patient had vertebrobasilar impairment. But the angiography findings were significant for occlusion of the lower third of the basilar artery. The study further highlights the importance of MRI and MRA in patients with acute onset bilateral hearing loss. This is because the hearing loss may be because of vertebrobasilar artery occlusive disease.
Case presentation
A 73-year-old Japanese woman presented to a local hospital with sudden-onset bilateral hearing loss with no signs of vertigo and vomiting. The patient’s medical history was significant for hypertension, hyperlipidemia, atrial fibrillation (AF) and CHA2DS2-VASC score (for atrial fibrillation stroke risk) of 3. On presentation, the patient was on medications including 5 mg of atorvastatin. After examination, doctors diagnosed her with sudden deafness and referred her to the emergency department. At this time her consciousness was clear.
Her family, social, environmental and employment history were insignificant. In addition, she had no history of smoking or alcohol. تنزيل العاب اون لاين On examination, her blood pressure was 147/72 mmHg, pulse rate of 78 beats per minute with AF and temperature of 36.8 °C. Her medical history revealed that a year before her presentation she had to stop her anticoagulant therapy because of recurrent episodes of epistaxis. She complained of only bilateral hearing loss without any signs of vertigo or vomiting. العاب الربح Neither were there any signs of Horner syndrome, dysphagia, diplopia, ataxia, weakness or dysarthria.
Investigations
Doctors referred her for computed tomography (CT) which showed no specific findings. She was sent home and was scheduled for audiometry the next day. According to the study, her consciousness decreased significantly the next day and she returned to the hospital. She was severely drowsy at the time of admission with a Glasgow Coma Scale (GCS) of 7, whereas the National Institute of Health Stroke Scale (NIHSS) score was 33. On examination, her blood pressure was 170/90 mmHg, whereas her pulse was 80 beats per minute and her temperature was 36.4°C.
Diagnosis and treatment
Doctors referred the patient for laboratory tests which showed a white blood cell count of “8.8 × 109/l, haemoglobin of 14.7 g/dl, platelet count 268 × 109/l, blood urea nitrogen 11.3 mg/dl, and creatinine of 0.58 mg/dl”. The patient’s liver function test results were also within the normal range. Doctors further advised diffusion-weighted imaging which showed acute multifocal lesions in the bilateral cerebellar hemisphere, pons and the posterior circulation. كيفيه لعب البوكر Magnetic resonance angiography (MRA) and 3D CT angiography (CTA) showed occlusion of the V3-4 segments, bilateral vertebral arteries and BA. However, because the conservative treatment was ineffective, doctors started the patient on edaravone infusion and performed endovascular treatment.
Transfemoral cerebral angiography showed occlusion of the V4 segment, proximal to its union with the BA. Angiography of the left common carotid showed retrograde blood flow into the BA and bilateral superior cerebellar artery (SCA) via the left posterior communicating artery. In addition, there was an obstruction in the proximal area, extending to the union area. Doctors attributed the patient’s sudden bilateral deafness to basilar artery occlusion. The study stated, “our patient had no symptoms of brainstem and cerebellar involvement. Among vascular causes, ischemic stroke in the territory of the AICA, a branch of the BA, is the leading cause of sensorineural hearing loss”.
Prognosis
The patient’s past medical history was significant for untreated AF. Similarly, the angiographic findings were consistent with cardioembolic thrombus-induced basilar artery occlusion. Doctors did not perform echocardiography. Treatment included endovascular treatment, however, her condition continued to worsen. The patient went into a coma, and brain CT showed a large brainstem lesion, obstructive hydrocephalus and massive cerebellar swelling.
“Many patients with vertebrobasilar occlusive disease have a poor outcome and experience truncal ataxia, quadriplegia, locked-in syndrome, coma, and death”. In this case, the patient’s delayed diagnosis was life-threatening. Therefore, it is very important for clinicians to consider the possibility of vertebrobasilar occlusive disorder in cases of sudden bilateral hearing loss. She passed away on the second day after admission. A whole body and brain autopsy were not performed.
Source: Journal of Medical Case Reports



