A 23-year-old woman suffered blunt force trauma. Subsequently, she underwent multiple surgeries before the surgeons could remove the retained wooden stick.
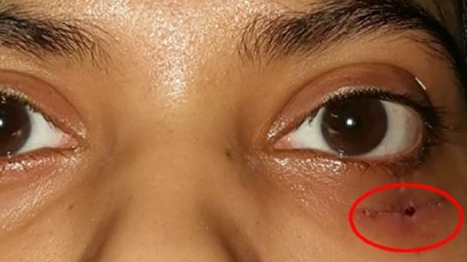
A 23-year-old Indian woman presented to a local hospital one week after suffering a blunt force trauma to her left cheek from a wooden stick. Initially, the trauma had resulted in local swelling. Also, there was a one-centimetre cut just below her left eyelid. When she visited the local hospital after a week, she also complained of discharge from the cheek wound.
In that hospital, the doctor performed minor surgery to remove the lodged wooden chip from her cheek. The doctor also prescribed her antibiotics. Although she completed the course, the cheek wound started discharging soon after she discontinued her medication. Therefore, she underwent a second surgery.
Eventually, she was referred to another hospital where they performed computed topography scan.
The patient said:
“My doctors went through the scan and said no foreign body was seen but told me that I will be taken for surgery to see my wound and also look for any residue of foreign body,”
During the third surgery, the surgeons removed more pieces of wood from the wound.
She added:
“A month later again I developed swelling over the same site but with a slight blurring of vision. I was very sad and went back to my doctor. This time my doctor was very sure of the foreign body and took me to the radiologist and told them about the certainty. I got my scan repeated, to my surprise my doctors said that the CT scan showed a huge foreign body inside.”
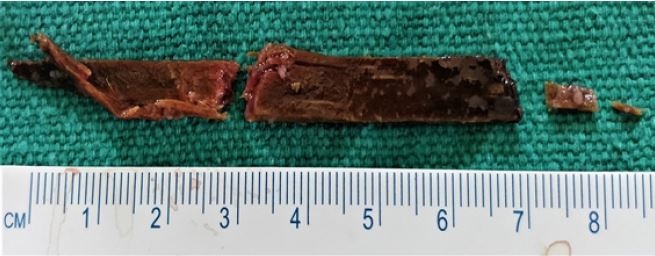
Fortunately or unfortunately, she underwent another surgery during which the surgeons removed a 7-centimetre long wooden stick from her cheek wound.
At the 2-month follow-up, the wound had healed well without any further complications.
She said:
“I’m really grateful to all my doctors whose insight and prompt decision helped me from losing my vision.”
This case particularly highlights the importance of thorough history, detailed examination, and timely diagnosis. After a blunt force trauma, a strong suspicion of a retained foreign body should always be considered. This is even more crucial when the patient presents with a history of orbital trauma.
In this case, since the patient had a retained wooden foreign body, the imaging studies were not able to detect as both the MRI and the CT scan can not detect wooden foreign body with 100% sensitivity. An early CT scan may miss a wooden splinter as it may become isodense due to water absorption. Ultrasonography is an alternative diagnostic method for identifying and localizing radiolucent foreign bodies
The most common complication in the management of soft-tissue foreign bodies is the failure to detect their presence, consequently, incomplete removal of the foreign body. It is imperative to remove the reactive foreign body, like wood, as early as possible to prevent complications. If not removed, it may cause inflammation, infection, toxic reactions, and granuloma formation.