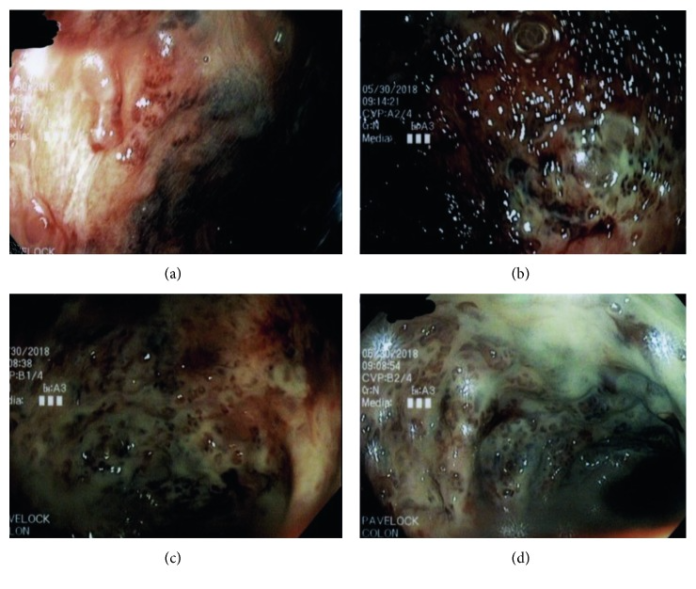
Secukinumab induced new-onset ulcerative colitis in 39-year-old male patient.
This article describes the case of a 39-year-old male patient with a rare case of new-onset ulcerative colitis induced by secukinumab. The patient had a medical history of psoriasis for which his dermatologist prescribed secukinumab. He presented with complaints of abdominal pain, bloody diarrhoea, fever and unexplained weight loss. The pain was in the suprapubic region associated with hematochezia and tenesmus which presented 6 months after presentation.
The patient’s medical history was remarkable of a 6-month history of severe plaque psoriasis. No other treatment worked, therefore, doctors advised secukinumab. His physician referred him to a gastroenterologist for evaluation of his symptoms of abdominal pain and fevers. Similarly, CT scan showed a few diverticula with no signs of active inflammation. Even though the initial colonoscopy was remarkable of mild inflammation of the sigmoid colon. His symptoms led to the diagnosis of infectious colitis. Doctors prescribed on ciprofloxacin and metronidazole. Although, there was no relief in symptoms.
Patient showed no improvement in symptoms even 5 days after initial treatment
He again presented to his local emergency department 5 days later with complaints of worsening abdominal pain, multiple loose bloody bowel movements in a day, chills and fever. Repeat CT showed thickening of the sigmoid colon. Doctors again prescribed an antibiotic treatment (piperacillin-tazobactam) with steroids for possible autoimmune colitis. Flexible sigmoidoscopy was remarkable of ulceration of the splenic flexure at 30 cm with moderate to severe active colitis in the rectum. However, there were no signs of inflammation past the transverse colon. Biopsy was remarkable of neutrophils within the crypts of lumen. Other findings included shortening of crypts and architectural distortion.
He remained admitted in the hospital for another 10 days. There was no improvement despite treatment. Therefore, doctors advised transferring him for further evaluation. His investigations were suggestive of bacterial infection. He continued passing blood-tinged stools with no improvements in abdominal pain despite steroids and was prescribed infliximab.
The findings led to the diagnosis of new-onset ulcerative colitis induced by secukinumab. The patient showed significant improvement two weeks after treatment after halting secukinumab.
References
A Rare Case of New-Onset Ulcerative Colitis following Initiation of Secukinumab https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6701396/