- Chromobacterium violaceum is a common cause of invasive diseases, including septicaemia in immune-compromised adults and neonates.
- There is a high risk of misdiagnosis which leads to poor outcomes.
- This case study highlights pleural empyema thoracis in a tertiary hospital in Nigeria.
This article describes the case of pleural empyema thoracis and urinary tract infection caused by Chromobacterium violaceum in a 31-year-old male patient. The patient presented to the emergency department with complaints of headache, anorexia and body weakness.
Examination showed tachypnea, the patient was febrile with respiratory rate of 40/min, heart rate of 98 beats/minute and blood pressure 110/70 mmHg. 2 months earlier the patient had presented with a history of an unproductive cough. The cough had an insidious nature and was intermittent in nature. He further complained of breathing difficulty, malaise and fever.
He had no history of coming in contact with a person with chronic cough.
Signs of orthopnoea and paroxsymal nocturnal dyspnoea were absent. The patient’s history revealed that the onset of his cough worsened with physical activities, for example, climbing the stairs which in addition caused difficulty breathing. The patient was also experiencing unexplained weight loss. Clinical examination was remarkable of an asymmetrical chest with reduced chest expansion and tactile fremitus on the left side of the lung. Chest auscultation revealed stony dulness and reduced vocal evidence in the left lung field, also. Other systemic examinations were normal, though.
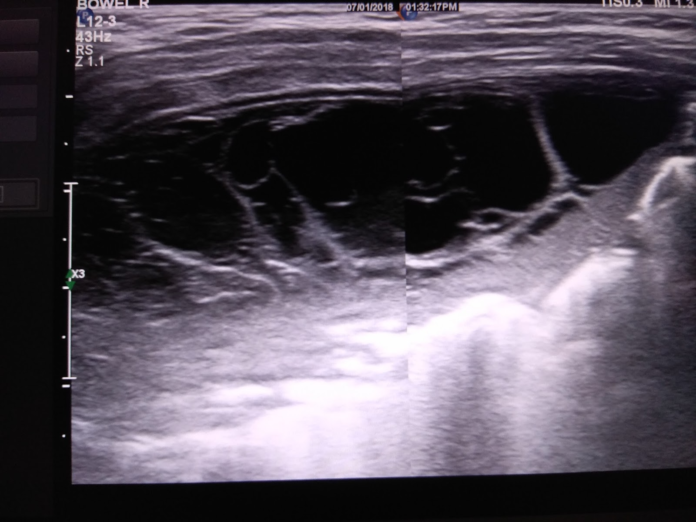
For further evaluation, doctors, advised chest radiograph which showed pleural effusion and deviation to the right in the trachea. Ultrasound scan showed a massive pleural effusion in the left lung with evidence of a lung abscess. Doctors diagnosed the patient with lobar pneumonia complicated with pleural effusion.
Treatment
Treatment included a closed thoracotomy tube drainage. 600 ml of pus was drained. Similarly, a Ziehl–Neelsen staining of the pleural effusion was negative for acid-fast bacilli. The findings were consistent with the diagnosis of empyema thoracis. Microbiology of the pleural empyema pus on Columbia blood agar showed a culture of C. violaceum. Doctors treated the patient with intravenous amoxycillin-clavulanic acid and ceftriaxone for seventy-two hours. However, the patient responded poorly to the medications. As a result, he was now given ciprofloxacin 200 mg 12 hourly for one week. He was discharged on clinical cure and treated with ciprofloxacin for one week as an outpatient.
References
Case Report on Pleural Empyema Thoracis and Urinary Tract Infection Caused by Chromobacterium violaceum from Lagos, Nigeria https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6383417/



