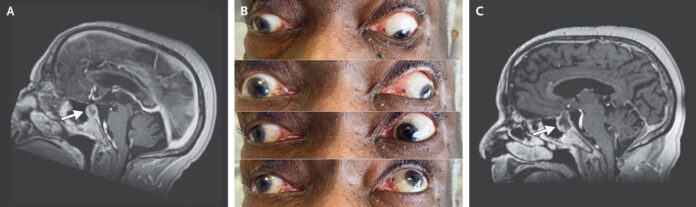
Sudden-onset headache and vision loss, patient diagnosed with pituitary apoplexy
An 81-year-old man arrived at the emergency room with a severe headache and vision loss. He had a nonfunctioning pituitary macroadenoma (Panel A, arrow) that had been monitored with serial imaging for the past four years. The right eye displayed ptosis, a nonreactive pupil, and paralysis of elevation, depression, and adduction on examination (Panel B), all of which were compatible with right oculomotor nerve palsy. There was also no light sensitivity in either eye. Central hypothyroidism and central adrenal insufficiency were discovered through laboratory tests. T1-weighted magnetic resonance imaging of the head indicated pituitary lesion growth with a new haemorrhage (Panel C, arrow). A pituitary apoplexy diagnosis was made.
Pituitary apoplexy is defined as sudden pituitary gland or tumour haemorrhage or infarction. It is characterised by severe headaches and may be followed by diplopia, visual loss, or hypopituitarism. Visual impairments are a sign that surgical decompression is necessary. Emergency endoscopic endonasal excision of the macroadenoma was performed after intravenous hydrocortisone was provided. The patient’s visual acuity recovered to normal on day four following the treatment. He was released from the hospital with instructions to continue taking prednisone and levothyroxine as maintenance medication. The right oculomotor nerve palsy had resolved after 3 months of follow-up.
Aetiology
Pituitary apoplexy is frequently associated with a pre-existing pituitary tumour. The majority of patients are completely unaware of the tumour. Endocrine stimulation tests, bromocriptine or cabergoline treatment, gonadotropin-releasing hormone treatment, lumbar fusion in the prone position, pregnancy, pituitary irradiation, anticoagulation, thrombocytopenia, and erectile dysfunction medications are all risk factors.
Sheehan syndrome develops in postpartum women who have pituitary gland necrosis as a result of ischemia following severe bleeding during childbirth. Adrenal insufficiency, hypothyroidism, and hypopituitarism are common symptoms, but visual alterations are uncommon. Because the gland did not have a pre-existing tumour, and visual symptoms are extremely infrequent, this condition is usually not classified as pituitary apoplexy.
Epidemiology
In cases of pituitary adenoma, the reported incidence of pituitary apoplexy ranges from 1.5 to 27.7%, but many studies do not differentiate between symptomatic and asymptomatic patients. When only symptomatic patients are considered, the incidence reaches 10%. The incidence rises to 26% when non-symptomatic intratumoral haemorrhage discovered by neuroimaging investigations is included. Apoplexy in pituitary adenomas is uncommon, occurring at a rate of 0.2% per year. Tumours greater than 10 cm in diameter, as well as those with rapid growth, are at a higher risk.
The majority of patients are between the ages of 37 and 58.The male-to-female ratio is close to 2:1.
Pathophysiology
Many of the symptoms are caused by haemorrhage, which causes an abrupt enlargement of the tumour. Direct compression of the optic nerves or chiasm causes visual symptoms, and hormonal dysfunction is produced by a sudden interruption in hormone flow.
Several hypotheses have been presented to explain the ischemia and hemorrhagic alterations observed in both the tumour and the normal gland. Although they are considered as separate mechanisms, it is likely that each theory contributes to some process, and the combination of them results in apoplexy. According to one idea, the superior hypophyseal artery and its branches are compressed against the diaphragma sella, causing ischemia of the anterior pituitary gland and tumour.
Another theory proposes that because the pituitary vascular network is constricted inside the narrow intrasellar compartment, it causes ischemia, necrosis, and haemorrhage. Finally, another idea holds that the tumour’s rapid growth outstrips its vascular supply, resulting in ischemia and necrosis.
Treatment
Immediate medical management of pituitary apoplexy patients comprises a careful assessment of fluid and electrolyte balance, hemodynamic stability, and corticosteroid supplementation. Even if they do not exhibit symptoms of adrenal crisis, all patients should be given corticosteroids. An intravenous 100-200 mg bolus of hydrocortisone is suggested. Continued administration of 50-100 mg every 6 hours is recommended. After the initial bolus, a continuous intravenous infusion of 2-4 mg/hour can be initiated.
The management of the mass is contentious, with some advocating early transsphenoidal surgical decompression in all patients, while others recommend a cautious approach for patients with normal consciousness and no visual acuity or field abnormalities.
Emergency surgery is recommended for more adverse symptoms
Patients with progressive deterioration of consciousness, hypothalamus involvement, and progressive visual impairment should have emergency surgery. It has been established that a surgical operation conducted as soon as possible results in significant postoperative clinical improvement. When visual acuity deficiencies appear stable, decompressive surgery can be delayed but conducted within one week. A cautious approach could be taken if the ophthalmoplegia is improving or stable. Endonasal or sublabial transsphenoidal surgery using a microscope is routinely employed. A craniotomy should be done to ensure total removal of very big tumours and those that extend over the chiasm or laterally to the temporal fossa.
Pituitary apoplexy can be effectively treated with endoscopic endonasal techniques. Endoscopic patients have a similar aesthetic outcome but a superior endocrinological outcome because the living tumoural component can be removed from restricted locations such as the cavernous sinus. An endoscopic method can be difficult to perform if it is required late at night since it requires the collaboration of an otolaryngologist and a neurosurgeon.
When compared to adults, paediatric pituitary tumour apoplexy has a more aggressive natural history, and early treatment may reduce its occurrence and improve prognosis.
Source: NEJM