Let’s imagine a hypothetical situation where a man walks into a coffee shop, climbs on top of a table and starts preaching to the people present. He claims he’s a prophet and that the end is near. After terrorizing the people for half an hour, he is escorted by the police to the local station. At the station, he is adamant about being a messenger of God and is only released after a family member provides the police with a doctor’s note stating him mentally unstable. The man is labeled a schizophrenic and he is released.
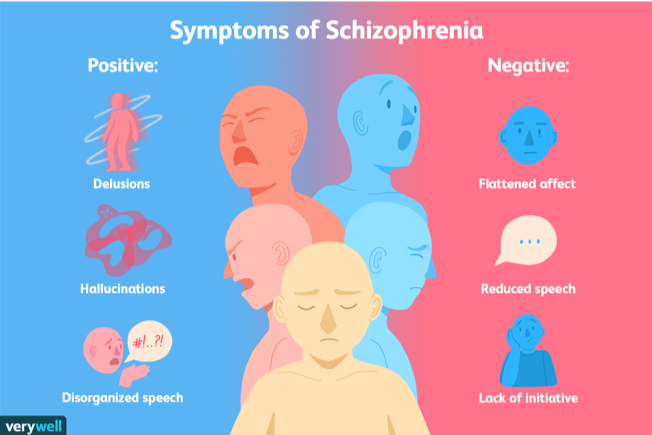
The papers are full of such cases where people have claimed to be God, abducted by aliens, being spied upon by the government and multiple other delusions. Delusions are one of the major symptoms of schizophrenia. Now, what is schizophrenia? Schizophrenia is defined as a mental disorder characterized by hallucinations, delusions, and disordered thinking. WHO’s International Statistical Classification of Diseases and Related Health Problems (ICD-10) states 7 subtypes of the disorder. Around 20 million people are affected by schizophrenia worldwide.
Schizophrenia is believed to be caused by a combination of factors ranging from genetics to psychosocial. In the early 1980’s it was hypothesized that dysfunctional synapses in the brain cause schizophrenia. In the nervous system, synapses allow for the transmission of signals between neurons.
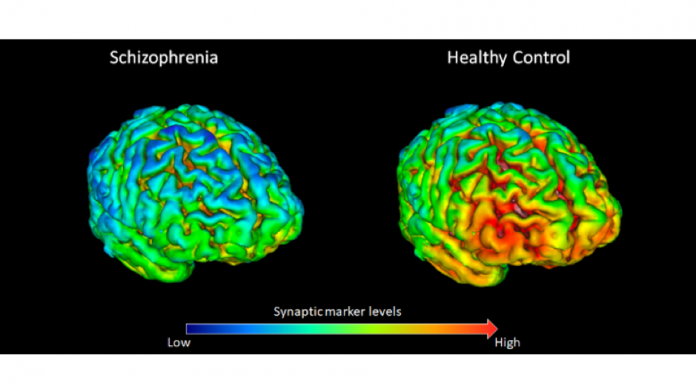
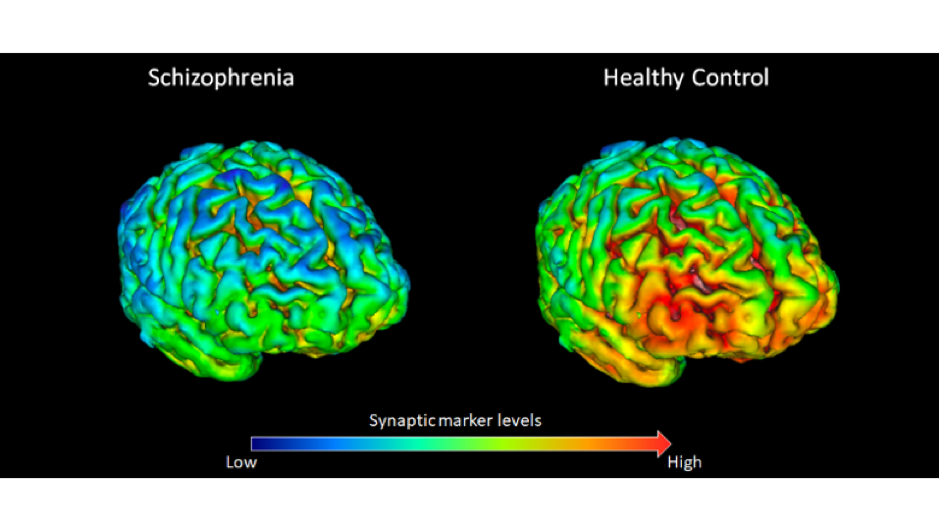
A recent study conducted by Imperial College London and King’s College London discovered lower levels of SV2A (synaptic vesicle glycoprotein 2A) in individuals with schizophrenia. After being injected with tracers that bind to SV2A, the patients underwent Positron Emission Tomography (PET) scans to produce a 3D image of the brain.
SV2A is involved in regulating vesicle exocytosis into synapses, causing the release of neurotransmitters. Insufficient levels of SV2A cause the synapses to lose their “connectivity,” which could be a key underlying factor in the development of schizophrenia. These lower levels were mostly seen in the frontal cortex which is the region of the brain involved in planning.
The current treatments for schizophrenia are very limited and according to Professor Oliver Howes, who led the study, this protein SV2A could be a target for new treatments to restore synaptic function.
The people with schizophrenia who were scanned had all received antipsychotic medication and to exclude this as a factor in the synaptic dysfunction, they gave antipsychotic drugs to rats for 28 days and found it had no effect on the levels of the protein SV2A. Thus, suggesting that antipsychotic treatments don’t lead to the loss of brain connections.
The researchers later hope to conduct this study on younger people, in the early stages of the disorder, to see how synaptic levels change during the development of the illness and whether these changes are established early on or develop over time.
References:
Onwordi, E.C., Halff, E.F., Whitehurst, T. et al. Synaptic density marker SV2A is reduced in schizophrenia patients and unaffected by antipsychotics in rats. Nat Commun11, 246 (2020). https://doi.org/10.1038/s41467-019-14122-0
https://www.who.int/news-room/fact-sheets/detail/schizophrenia
https://www.who.int/classifications/icd/en/GRNBOOK.pdf