Case Presentation
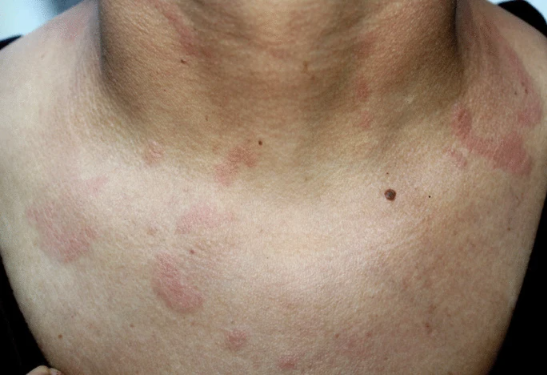
A 38-year-old North African woman presented to the Nephrology department due to a complaint of swollen legs for a month. She had a history of an underactive thyroid and had been unable to conceive for a year. Furthermore, she also complained of tiredness and had lost 3 kilograms in one month. She did not have a fever, joint pain, or muscle pain. However, she mentioned that she had developed patches on her skin that were sensitive to light, had fine scaling, and were itchy.
Examination
During the examination, doctors found that her blood pressure was 110/70 mmHg, her pulse rate was 99 beats per minute, her temperature was 36.3 °C, and her breathing rate was 18 breaths per minute. The skin examination revealed raised red patches on her neck, face, and chest, as well as swelling in both of her lower legs. The skin patches did not show any signs of scarring or changes in color. Initial laboratory blood tests showed a low level of albumin. A microscopic examination of her urine revealed the presence of red and white blood cells, along with protein.
Investigations
Electrophoresis showed an abnormal increase in a protein called gamma globulin. Her creatinine level was within the normal range. Moreover, the white blood cell count was normal. Her haemoglobin level was 12 g/dL, and her platelet count was 178,000/mm3. Antibody tests showed positive results for several autoimmune antibodies. The levels of certain complement proteins, which are involved in immune responses, were low. Additional tests for other antibodies and immune markers were negative. Doctors performed a skin biopsy that confirmed the diagnosis of a condition called lupus erythematosus tumidus (LET). LET is a disease characterized by inflammation and abnormal deposits in the skin and is a form of SLE.
The doctors performed an ultrasound of the patient’s kidneys, and they found that they were normal in size. However, they proceeded to perform a biopsy of the kidney. When the doctors examined this tissue under a microscope, they discovered that 8 out of the 34 kidney glomeruli were scarred, while the rest showed some deposits and infiltration of neutrophils. They also discovered that the glomerular basement membrane was thickened in some areas. The tissue between the kidney tubules had some signs of inflammation, and the tubules themselves showed small areas of damage and deposits of protein and red blood cells. The small arteries in the kidney had an increased amount of fibrous tissue. Tests for amyloidosis came back negative. When the doctors examined the tissue under fluorescent light, they found that certain proteins were present in abnormal amounts in specific areas of the kidney.
Diagnosis: Lupus Erythematosus Tumidus
Based on the patient’s symptoms and test results, she met six criteria for the diagnosis of systemic lupus erythematosus (SLE). The patient received treatment for proteinuria using ACE inhibitors, and she also received corticosteroids and hydroxychloroquine for the symptoms of SLE. After one month of treatment, her skin lesions improved. At the 6 and 12-month follow-up appointments, the amount of protein in her urine decreased. At the final follow-up, which was 22 months after her initial presentation, her proteinuria had decreased further, her kidney function was normal, and her skin lesions had completely resolved.
Discussion: Lupus Erythematosus Tumidus
Lupus erythematosus tumidus (LET) is a rare chronic skin disease characterized by inflammation. LET is usually found with systemic lupus erythematosus (SLE) in some cases. The skin lesions in LET can be divided into two categories: SLE-specific and non-specific. LET primarily affects areas of the skin that are exposed to the sun, appearing as red, swollen patches that do not leave scars.
The progression from LET to SLE has been reported in 12% to 18% of cases. The relationship between SLE and LET is not fully understood, and only a few cases have been reported, most commonly in Europe.
This case is unique since the patient is from North Africa, while most reported cases come from other regions. Most LET patients have negative anti-nuclear antibody (ANA) results, with ANA positivity seen in less than 20% of patients. The presence of other antibodies seen in systemic lupus, such as dsDNA, SSA, SSB, or low C3 and C4 complement levels, is rarely observed in LET. Although systemic symptoms are not commonly observed in LET patients, there has been a case where systemic symptoms developed during the disease. LET has also been reported to occur in the course of Systemic Sclerosis.
This case is also significant because it involves the rare association between LET and severe SLE with lupus nephritis (NL).
Treatment for LET typically involves hydroxychloroquine sulfate, with a daily dosage of 6–6.5 mg/kg. Systemic corticosteroids or immunosuppressants are not usually used, but they were prescribed in this patient’s case due to the diagnosis of lupus nephritis. Photoprotection is important for LET patients due to their high sensitivity to sunlight.