A 47-year-old businessman undergoes multiple investigations for a long-standing complaint of bad breath.
A 47-year-old, otherwise healthy, businessman presented to the outpatient department with complaints of bad breath since long. Although the complaint was long-standing, the patient felt a recent increase in the symptom. The patient had tried all the over-the-counter remedies. Some of them produced little benefit, but overall, the treatment efforts ended in smoke.
He had visited to multiple dentists and oral hygienists, but the visits remained unfruitful.
He did not have any other complaints. Moreover, past medical history was unremarkable. He was not aware of nor diagnosed with gastroesophageal reflux disease or indigestion. Social history revealed that he consumed no more than 20 units of alcohol per week. Additionally, he was a non-smoker. His diet was varied, with an occasional takeaway or other ‘convenience food’.
Examination:
Physical examination revealed a healthy male who was well oriented and aware. His BMI was 24kg/m2. Examination of the oral cavity was unremarkable. However, he had a mild, albeit noticeable, putrid odour. The rest of the examination remained unremarkable.
His dentists had prescribed him antibiotics to treat any potential underlying sinus infection. So the patient had completed two courses of antibiotics including erythromycin and doxycycline. However, the medications did not benefit him.
Serological investigations revealed normal full blood count, liver function tests, renal profile, blood sugar, inflammatory markers, and amylase. However, the C-reactive protein levels were mildly elevated (23 mg/dL) and the gamma-glutamyl transpeptidase level was 55IU/L.
Stool test for Helicobacter pylori was also normal. However, the doctors prescribed him a trial of Proton Pump Inhibitors (PPIs).
Moreover, the doctors counselled the patient to reduce his alcohol intake as he might be unintentionally underestimating the amount of alcohol he is consuming.
PPIs yielded no positive results; the doctors referred the patient to the ENT specialist for further assessment. They suspected a pharyngeal pouch, which was confirmed by the barium swallow.
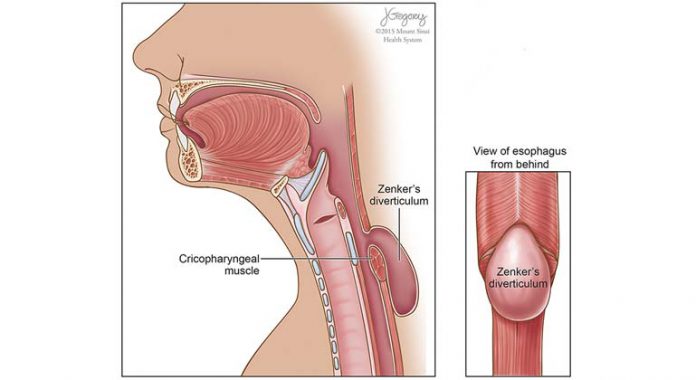
The patient received a diagnosis of Zenker’s diverticulum.
Zenker’s diverticulum
It is a hypopharyngeal diverticulum which out pouches due to weakened muscles between the thyropharyngeal and the cricopharyngeal muscle, the pharyngoesophageal junction. It has a 1.5-fold male predominance with patients presenting mostly in the middle- or old age. Patients may present with complaints of progressive, regurgitation of undigested food, chronic cough, aspiration (increased risk of aspiration pneumonia), halitosis, a sensation of a lump in the throat, and hoarseness. The swelling of the pouch may be visible or palpable in some patients.
Barium swallow is the mainstay of diagnosis.
The management can be according to the size of the pouch. Smaller pouches can be managed conservatively, while larger ones require surgery.
This patient opted for surgery. The surgeons performed a simple myotomy. Thereafter, his symptoms resolved, and he recovered well.