Case Presentation
A 74-year-old woman who had undergone remote percutaneous coronary intervention for coronary artery disease (CAD) in 2014 and had degenerative lumbar spine spondylosis status post-PVP in April 2021 presented to the emergency room with chest pain and shortness of breath that had persisted for two days (September 2021).
Investigations
On admission, the electrocardiogram revealed new diffuse ST segment depression with a significant rise in troponin levels over 3 hours from 32 to 672 pg/ml (typical reference: 0–10 pg/ml). Non-ST segment elevation myocardial infarction was identified as the cause.
The patient underwent an urgent left heart catheterization (LHC), which indicated diffuse calcified CAD with small-vessel disease as the cause of the patient’s clinical presentation, and medical therapy was determined to be the best option. Moreover, a mobile radiopaque non-coronary structure appeared on fluoroscopy over the projected area of the right atrium (RA), representing a new interval finding compared to the patient’s previous LHC performed almost a year previously (September 2020) when the patient presented with similar symptoms.
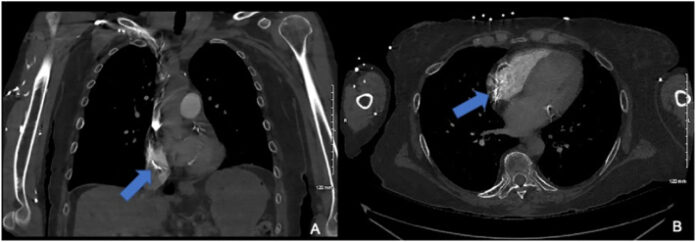
Moreover, transthoracic echocardiography (TTE) detected a floating foreign body in the RA that extended caudally into the cranial end of the inferior vena cava (IVC). A computed tomography (CT) scan revealed a foreign body in the right heart but no signs of pulmonary emboli.
Invasive Procedure
Following a multispecialty discussion, interventional radiology services used an endovascular method for foreign body retrieval. Under ultrasound guidance, an endovascular approach was conducted through the right common femoral vein. A 10-French sheath was advanced over a wire to the IVC, followed by a gooseneck snare and entangle device. A linear looping foreign body in parts was successfully extracted from the cranial end of the IVC.
Pathologic evaluation of the 1x 0.5x 0.5 cm hard foreign body confirmed that it was made of bone cement, which was compatible with an intracardiac bone cement embolism following a recent PVP that the patient had five months before her index presentation.
Discussion
Intracardiac cement embolization (ICE) is a rare complication of percutaneous vertebroplasty (PVP), which should be taken carefully as severe cardiac events have already been recorded previously.
The size of cement emboli often ranges from microscopic pieces to bigger particles, which can cause arterial blockage or interfere with valve function, and cause serious hemodynamic compromise.
Some risk factors for ICE after PVP have previously been reported. Instrumentation of the thoracic vertebrae, the presence of spinal metastases, and a greater number of instrumented vertebrae at the same session were all linked to an increased risk of ICE.
The majority of the cases examined required operational management to remove the cement emboli. In one case, a robotic-assisted endoscopic right atriotomy was used, and an endovascular technique was successful in another. Each case was managed with a different approach depending on the patient’s condition and the physician’s level of expertise
However, patients who had cement-induced atrial or ventricular wall perforation with pericardial effusion deserved immediate surgical intervention.