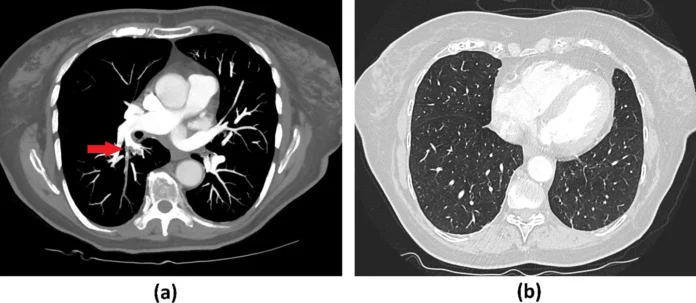
This case is of a 71-year-old female with ovarian cancer undergoing first-line chemotherapy presented with pain in her lower left leg with progressive dyspnea. Moreover, her general practitioner had already prescribed her dabigatran for deep vein thrombosis a day before her admittance.
History of Treatment for Ovarian Cancer
The patient was going through multimodal treatment for HGSOC FIGO IIIC. She underwent complete macroscopic tumour resection, in addition to bilateral adnexectomy, peritonectomy, hysterectomy, pelvic and paraaortic lymphadenopathy, omentectomy, rectosigmoid resection and partial liver resection.
Her doctors initiated her first-line chemotherapy with carboplatin AUC 5 and paclitaxel every three weeks. After her first course completion, they switched to weekly carboplatin AUC 2 application and paclitaxel for better tolerability. Since the patient had delayed wound healing, doctors postponed the initiation of bevacizumab. The patient was in a good state otherwise and had complained of general weakness only.
Medical History
She had a history of treatment for papillary thyroid cancer by total thyroidectomy and catheter ablation of AV node for atrioventricular nodal reentry tachycardia. Her gynae and obstetrical history were uneventful and her BRCA was negative. Moreover, she had no family history either. She didn’t smoke, or drink and was taking pantoprazole, L-thyroxin, and vitamin D regularly.
Clinical Examination
Clinical examination was normal with chronic anaemia and elevated infection parameters. Renal and hepatic functions were also normal, however, sonography revealed mild urinary stasis on the left side.
Colour Duplex sonography confirmed deep vein thrombosis of the right gastrocnemius muscle vein. Furthermore, chest CT revealed segmental PE in one artery centre of the lung and in multiple subsegmental arteries. Although there were no changes for COVID19, her nasopharyngeal swab test was positive with SARS-CoV-2 via reverse transverse polymerase reaction testing. Since there was no sign of right heart overload, doctors continued the treatment with LMWH and compression stockings.
The patient quarantined at home and anticoagulant treatment continued with apixaban for 6 months. A therapeutic gap of 5 weeks was given, and her chemotherapy was resumed with a weekly regimen. Moreover, urinary stasis causing lymphocele of the left lower abdomen was drained without any complications after five months; followed by maintenance oncological therapy.