- The hump-nosed pit viper (HNP) is a moderately venomous snake.
- HNP snake bites are a common occurrence in Sri Lanka and South India.
- This case highlights an atypical clinical manifestation of a hump-nosed pit viper bite.
This article describes the clinical manifestation of hump-nosed pit viper bite in a previously healthy 47-year-old female. The patient belonged to the Kegalle district, in Sri Lanka. As per her, she was bit by the snake near the back door of her home. Similarly, right after she was bit, there was heavy bleeding at the site of the snake bite. A few minutes after being bit, the patient felt dizzy, nauseated and was screaming in pain because of the bite. In addition, her entire body was numb with profuse sweating and salivation.
While she was being taken to the hospital, her limbs became right and she clenched her jaw tightly. She was unresponsive for a good 5 minutes and frothing which indicated a generalised seizure. She was at the hospital after 30 minutes. The doctor in the outpatient department referred her to the internal medicine ward for administration of antisnake venom.
Physical examination
Physical examination was remarkable of a pulse rate of 100 beats/minute and blood pressure 150/90 mmHg. However, the lungs were clear on auscultation with oxygen saturation of 95% while the patient was breathing ambient air. She had no neurological deficit either. By this time residents of the area has killed the snake and brought it in to the hospital. Doctors identified the snake as a hump-nosed pit viper. Therefore, doctors advised against administration of antisnake venom.

Further investigation showed that her blood clotting time, platelet count, prothrombin time and international normalized ratio, and activated partial thromboplastin time and liver function were all normal. Despite bleeding at the site of the bite even on admission. Arterial blood gases were indicative of a compensated metabolic acidosis. On the 2nd day, doctors transferred her to a different hospital for further management.
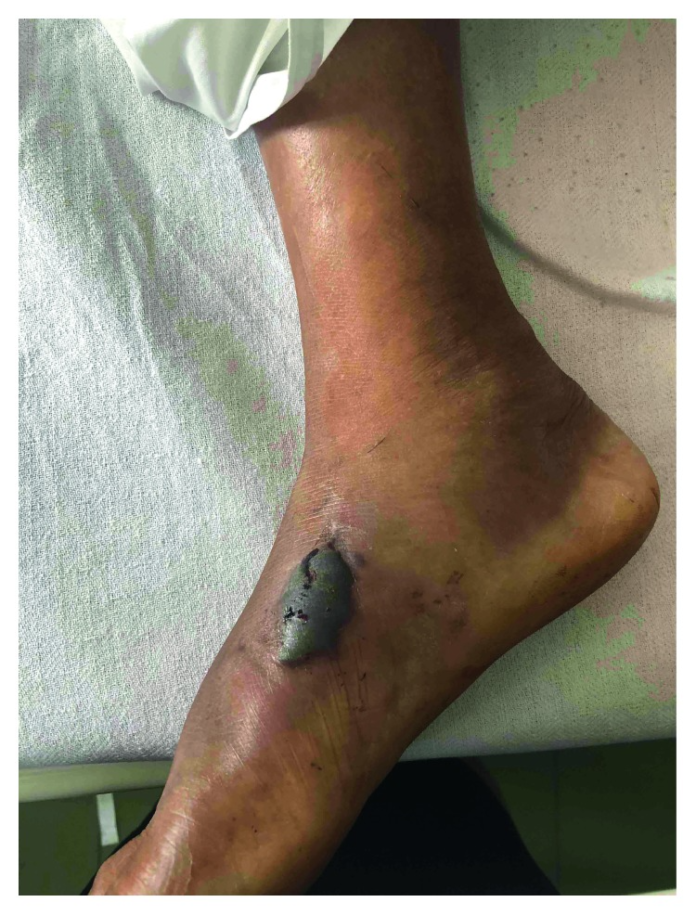
On the 2nd day of admission, a bulla developed at the site of the bite with oedema and warmth at the right foot. Lab work showed neutrophilic leukocytosis and increased CRP level. Doctors started the patient on intravenous antibiotics to cover the wound infection. Her serum creatine was elevated with presence of oliguria on the 2nd day of admission. However, her serum sodium and potassium levels were within normal range from the 1st to the 5th day.
Management
Doctors started her on hemodialysis on the 2nd day, for every other day with fluid management. This continued for 24 days. In addition, doctors started her on oral sodium bicarbonate. The nephrology team managed her for acute kidney injury.
On the 3rd day, the patient’s blood pressure increased to 160/90 mmHg. Doctors prescribed prazosin and nifedipine SR to control the blood pressure. However, her blood pressure remained 140/90 mmHg high till she was discharged. She also developed bilateral lung crepitations that remained for the next 7 days. Moreover, parotid swelling and oedema of the right leg developed on the 3rd day which lasted for 3 days. The oedema lasted for 10 days. There were no signs of hemolysis on the blood work taken on the 2nd day. Although, on the 5th and 11th day her blood work showed microangiopathic hemolytic anemia.
She was referred to a consultant of transfusion medicine who performed plasmapheresis on her on the 7th day. In addition to four other cycles of plasmapheresis with regular wound toilets and debridements. The investigations that followed including EEG were all normal.
References
An Atypical Clinical Manifestation of a Hump-Nosed Pit Viper Envenomation https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6470431/