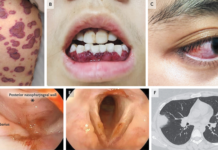
No, this picture is not of a pregnant uterus, neither of triplets or quadruples, infact, here uterus is not the culprit, it’s the ovaries!
This case is of benign ovarian cysts in a young, overweight female who was in her early 20s at the time of presentation with complaints of increasing abdominal girth and weight gain, for which she initially blamed her overweight body and diet, thus a 6 months’ delay in seeking medical attention.
Abdominopelvic Ultrasound and CT scan revealed huge cysts in both ovaries which were later diagnosed to be cystadenoma and teratoma in her left and right ovaries respectively.
Shown above, is a pre-operative image of the patient’s abdomen when she was carrying a 33 Kgs (72 pounds) heavy cystadenoma in her left ovary and a 10×10 cm teratoma in her right ovary for 11 months!
Ovarian tumors are classified1 according to the tissue of origin, with epithelial tumors being most common (65%), others include germ cell (15%), sex cord-stromal (10%) tumors. Epithelial tumors are further classified according to cell type and malignant potential. Case in discussion here had a ‘cystadenoma’ which is a benign epithelial tumor, and a ‘cystic teratoma or dermoid cyst’ which is a germ cell tumor, in left and right ovaries respectively.
The irony of ovarian masses is that these are either asymptomatic or present with vague symptoms such as pelvic pain, pressure, bloating, abdominal discomfort and sometimes, menstrual irregularities, hence the delay in diagnosis, in fact, most ovarian masses are identified incidentally on ultrasound. The disadvantage of malignancies being diagnosed at an advanced stage is that only palliative care can be offered, unlike benign masses which have wider door to treatment options. Depending upon certain factors such as: age, size of mass, risk factors for ovarian cancer, family history, fertility requirement etc. either cystectomy or oophorectomy can be performed, while former is the procedure of choice when fertility is desired and the mass is smaller in size, the latter is strongly advised when malignancy is suspected. Moreover, special attention must be paid to minimize the potential for tumor dissemination during surgery. لعب قمار حقيقي Non-surgical treatment or watchful waiting is for women with either physiological cysts, which resolve spontaneously or for those with lower malignant potential; such women can be followed with serial ultrasound and tumor markers-but neither ofthe two has been proven to bethe best surveillance approachtill date.
A noteworthy point here is that with hugemasses like theone mentioned in theabove case, thereare higher chances oftorsion. Suchpatient presents with acute pain which is to be urgently exploredand operated,onlyafter excludingan ectopic pregnancy. Other complications include rupture orhemorrhagewithin the cystwhich aremanaged accordingly. موقع قمار
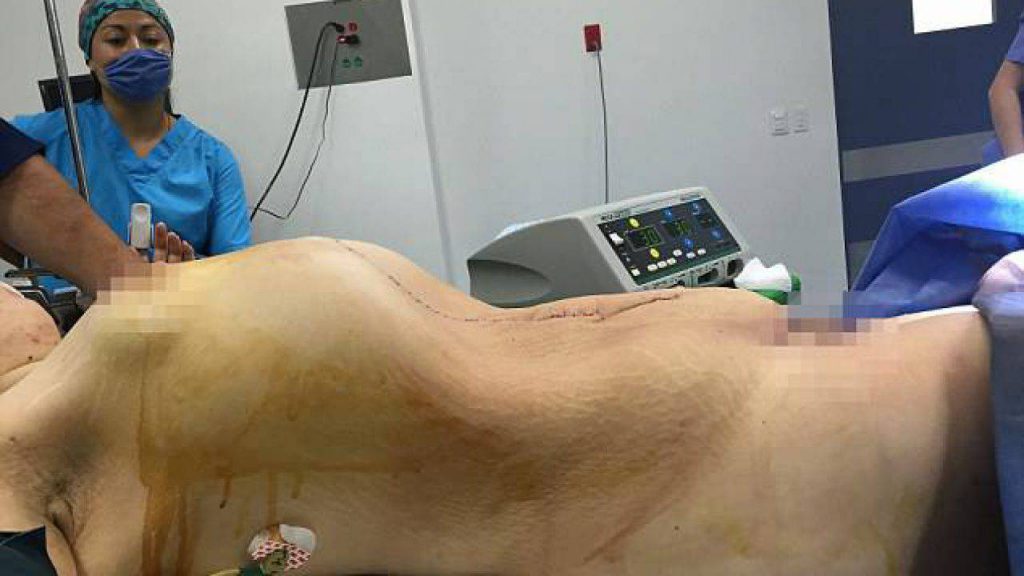
In the above mentioned case, cystectomy was not advisable therefore laparotomy was performed to remove both ovaries (bilateral oophorectomy). مواقع الرهان على المباريات No complications were observed postoperatively(image shown below), therefore she was discharged after routine medical care.
References
1 (n.d.). Retrieved from https://www.pathologyoutlines.com/topic/ovarytumorwhoclassif.html
Ehdaivand.S. (n.d.). WHO Classification. Retrieved from www.pathologyoutlines.com/topic/ovarytumorwhoclassif.html
2 Limaiem F, Mlika M. Ovarian Cystadenoma. [Updated 2019 Nov 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK536950/
3 Muto, M. G. (n.d.). Retrieved from uptodate.com:
4 Muto, M. G. (n.d.). Retrieved from uptodate.com: