69-year-old suffers from broken heart syndrome after sister’s death
This article describes the case of a 69-year-old female patient diagnosed with broken heart syndrome, also known as stress-induced cardiomyopathy or Takotsubo cardiomyopathy. Broken heart syndrome presents symptoms similar to acute myocardial infarction, however, without coronary artery stenosis. In terms of management, there are significant differences between Takotsubo cardiomyopathy and acute myocardial infarction.
The patient presented to the emergency department with complaints of dizziness, malaise and a pre-syncope attack. The symptoms presented after she experienced intense emotional stress after her sister’s death. The patient’s medical was significant for hypertension. There were no signs of chest discomfort, dyspnoea or retrosternal pain. She was taking aspirin and valsartan.
On examination, the patient’s vital signs were normal. Doctors advised a twelve-lead standard electrocardiogram which revealed normal sinus rhythm with a slight elevation in the ST-segment of about 1 mm in V1-V3. Similarly, biphasic T wave changes were also evident in V1-V4. Further routine laboratory tests were performed, including complete blood cells, liver function tests, electrolytes and lipid profile. All test results were within normal limits. However, an elevation was evident in cardiac enzymes. Doctors transferred the patient to the catheterization laboratory where a coronary angiography was performed. The findings of the coronary angiography showed non-obstructive plaques at the left anterior descending artery and proximal part of the circumflex artery (LCX).
The patient was diagnosed with minimal coronary artery disease
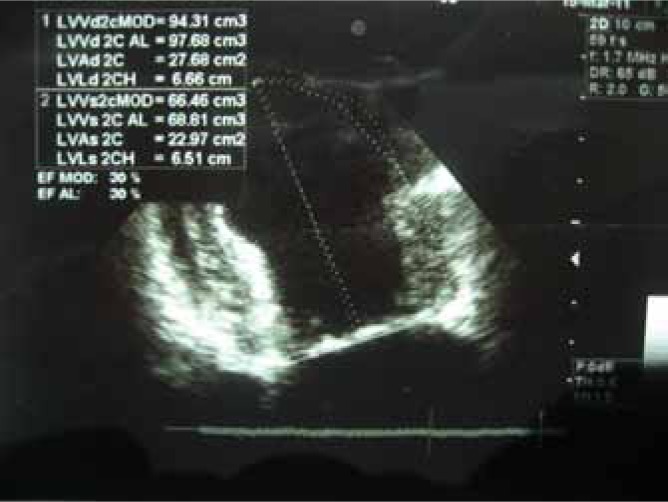
Doctors diagnosed the patient with minimal coronary artery disease based on the findings. For further evaluation, a left ventriculography was performed which showed akinesia at the mid-inferior, mid-anteroseptal and apical segments of the left ventricle. In addition, left ventricular injection was significant for severe systolic dysfunction. Treatment included beta-blockers, diuretics, Clopidogrel, Aspirin and angiotensin converting enzymes.
The patient was discharged after 5 days with no further complication during the hospital course. Similarly, doctors advised her to get reevaluated after a month. Follow-up visit showed that all her symptoms had disappeared. Repeat echocardiogarphy showed improvement in left ventricular systolic function with a normal ejection fraction.
Broken heart syndrome was initially reported in Japan with subsequent cases in USA and Europe. The term Takotsubo is Japanese for narrow-narrow necked octopus trap, resembling the apical ballooning configuration of the left ventricle in systole. The pathophysiology of the disease is transient systolic dysfunction of apical or mid segment of the left ventricle in the absence of obstructive coronary disease. It is more commonly seen in postmenopausal women with a mean age of 61-76 years, as in this case.
References
Broken Heart Syndrome: A Case Report https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3524327/



