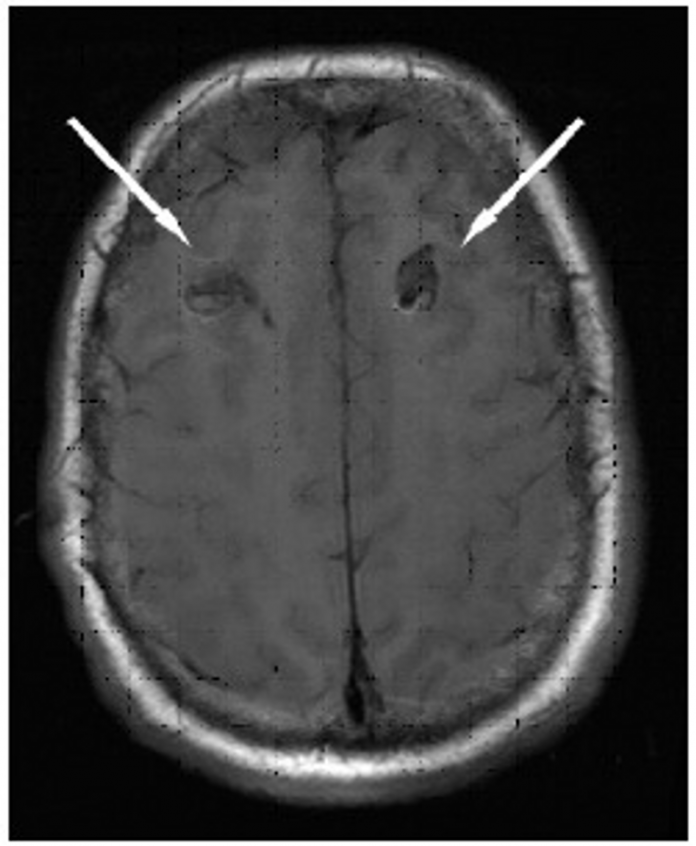
A 56-year-old male patient was brought to the emergency with altered mental status. He was diagnosed with a brain abscess caused by untreated tooth caries.
A 56-year-old male patient presented to the emergency with a brain abscess caused by untreated tooth caries. The patient was brought to the hospital by his coworker because he arrived at work looking unwell and with an altered mental status. The patient had a medical history of hypertension, cholecystectomy and obstructive sleep apnoea. He was recently prescribed lisinopril for dry cough, in addition to losartan and furosemide for his sleep apnoea.
During this time the patient developed an intermittent fever. Moreover, a week before presentation, he experienced a memory lapse of recent events and tunnel vision. Over this time period, he also experienced constant headaches that grew worse with time. Five days before he presented to the emergency, he developed pain in his neck and back associated with nausea and vomiting. Six months earlier, he even complained of a tooth ache on his left side that subsided without any treatment.
For further evaluation, the patient was advised a CT scan which showed multiple intracranial mass effect lesions and hydrocephaly.
The differential diagnosis included brain abscess and neoplasm
The patient was prescribed vancomycin, aciclovir and ceftriaxone and was transferred to a level 1 trauma centre for advanced care. Physical examination showed that his pupils were sluggish, non-reactive and miotic. Similarly, nuchal rigidity was unclear. The patient was prescribed fuconazole and aciclovir and lisinopril were discontinued.
Cerebrospinal fluid samples showed an elevated white blood cells count and protein. MRI and CT ruled out peripheral neoplasm and confirmed unchanged intracranial lesions of mass effect. two days after admission and abdominal CT was performed which showed a metallic similar to a dental filling in his abdomen that had not been seen in previous scans.
The diagnosis of brain abscess was confirmed following a craniotomy of the right temporal lesion. Histopathology of the brain biopsy and exudates showed gram-positive anaerobic streptococcal species, commonly associated with dental infections. An oral aetiology was suspected and CT scan of the maxillofacial region showed grossly decayed first and second upper molars. Radiographic evidence showed periodontal abscess involving the maxillary sinus.
The patient was diagnosed with gross caries, necrotic pulp and chronic periapical abscess of upper right first and second molars
Both decayed molars were extracted and ceftriaxone was continued. He was placed on external and ventricular drains. He stayed in the hospital for 44 days and was discharged to a skilled nurse facility with the following prescription medications: mlodipine, clonidine, famotidine, heparin, levetira-cetam, metoprolol, modafinil, nystatin powder, salt tablets, valsartan, vitamin D and ceftriaxone. After complete recovery he was asked to continue ceftriaxone for 14 days.
References
A case of odontogenic brain abscess arising from covert dental sepsis https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3954226/