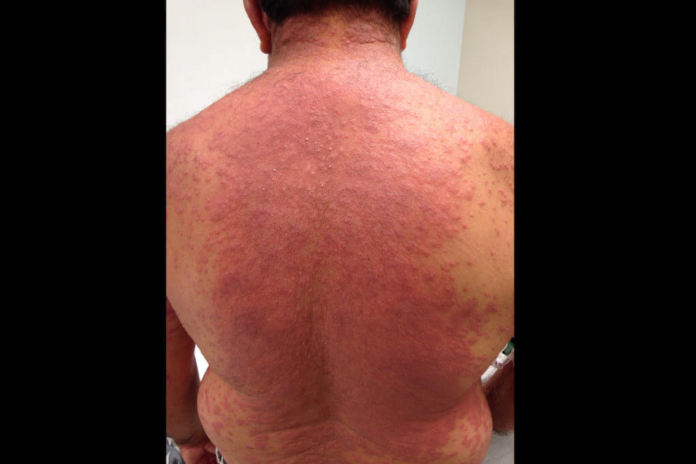
DRESS syndrome
This article describes the case of a 62-year-old male patient who presented to the emergency with complaints of a 4-day history of abdominal pain, rash, fever and lymphadenopathy. His medical history revealed obesity, gout and hypertension. The patient also hadThe patient had been hospitalised for gout, five weeks ago, for which the doctors prescribed allopurinol. The clinical and investigation findings led to the diagnosis of DRESS syndrome.
Physical examination showed fever and a rash covering 60% of the total surface area of the body. In addition, there were signs of cervical, axillary and inguinal lymphadenopathy and right upper quadrant tenderness on palpation. Laboratory workup was significant for leukocytosis and eosinophilia with elevated level of alanine aminotransferase. Similarly, histopathology showed foci or interface dermatitis and perivascular lymphocytic infiltrates. Based on the findings, doctors diagnosed the patient with Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome.
The syndrome is an acute dermatologic emergency. Likewise, it is a rare syndrome that differs from adverse drug reactions in its idiosyncratic presentation, systemic organ involvement, mortality rate and time of onset in relation to the offending agent.
New cutaneous and systemic reactions were reported with the development of phenytoin, a novel pharmaceutical agent at the time.
The drug triggered several symptoms including lymphadenopathy, eosinophilia and fever that emerged several weeks after the drug’s initiation. Similarly, the drug-related syndrome was referred to as anticonvulsant hypersensitivity syndrome, drug-induced delayed multiorgan hypersensitivity syndrome and phenytoin/Dilantin syndrome. The precise pathogenesis of the syndrome is unknown, however, there are several mechanisms that are considered as contributory mechanisms. The most common drugs implicated for DRESS syndrome are anticonvulsants.
The syndrome typically presents as a febrile rash with lymphadenopathy and eosinophilia, as in this case. Treatment includes stopping the offending drug, supportive care and steroids.
References
Large, Spreading Rash After Illness https://www.clinicaladvisor.com/home/dermatologic-look-alikes/large-spreading-rash-after-illness/