Sore throat is considered a seasonal disease by a majority
of us. Mostly, mild soreness takes its time and fades away, while moderate to
severe ones require treatment with antibiotics.
But can sore throat have long term complications?
Can sore throat lead to another condition even after its
resolved?
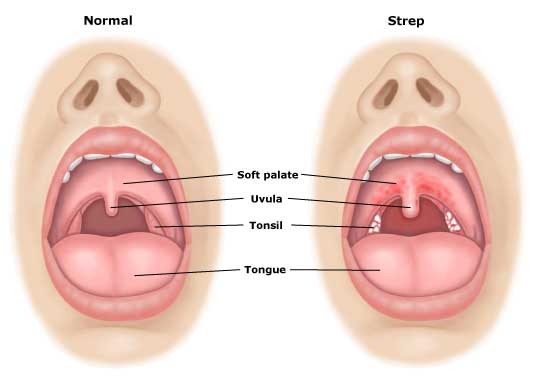
A 47-year-old man was diagnosed with pharyngitis when he
complained of sore throat and fever for which he was started on penicillin V
potassium. A week later, he presented to the emergency department with complaints
of pustular rashes on both of his hands.
Given his history of pharyngitis, a throat swab was taken to
detect the organism. The culture grew group A β-hemolytic streptococcus.
On examination, the palms of the hands and the soles, bilaterally,
had multiple pustules surrounded by an erythema. The rest of the examination
was normal. The joint examination was also unremarkable. موقع مراهنات
Serology revealed an absolute neutrophil count of 14,900
per cubic millimeter and a C-reactive protein level of 30 mg per liter. Renal
function test was normal.
Histopathological evaluation of the punch biopsy of a palmar
lesion showed a subcorneal pustule and mononuclear-cell infiltrates in the
dermis.
A diagnosis of post-streptococcal pustulosis was made.
Treatment with topical clobetasol was initiated. The rash
resolved in 14 days. At 1-year follow-up, the patient had no recurrence of the
rash or any long term complications of streptococcal pharyngitis.
Poststreptococcal pustulosis is quite a rare postinfectious
disorder secondary to streptococcal pharyngitis. Its rarity can be advocated by
the fact that only
25 cases have been reported worldwide.
Although it can involve the whole body, it typically starts
with a bilateral and symmetric eruption of pustules predominantly on the hands and
feet with high leukocyte count and elevated C-reactive proteins and other
acute-phase reactants. Other complications of post-streptococcal pharyngitis
may include arthropathy and glomerulonephritis.
Poststreptococcal pustulosis resembles palmoplantar
psoriasis, acute generalized exanthematous pustulosis, pustular psoriasis, pustular
vasculitis, and subcorneal pustular dermatosis; therefore, high chances of a
misdiagnosis.
Correct diagnosis and early treatment are imperative to
avoid any long term complications.
References
Tal Goldberger, M. a.-P. (2020, August 20). Poststreptococcal Pustulosis. Retrieved from The New England Journal of Medicine https://www. مراهنات رياضية nejm.org/doi/full/10.1056/NEJMicm2002486
Auer-Grumbach P, Pfaffenthaler E, Soyer HP. Pustulosis acuta generalisata is a post-streptococcal disease and is distinct from acute generalized exanthematous pustulosis. سلوتس Br J Dermatol. 1995;133(1):135-139. doi:10.1111/j.1365-2133.1995.tb02508.x
Fleming P, Shaw JC. Cyclosporine in the Management of Poststreptococcal Pustulosis. JAMA Dermatol. 2015;151(3):345–346. doi:10.1001/jamadermatol.2014.3517




