A new device to test cancer drugs on multiple tumor cells to improve cancer management.
One of the biggest challenges in treating cancerous is to stop the uncontrolled growth and unregulated multiplication of the cancerous cells. Some of the chemotherapeutic agents have succeeded in slowing or stopping the rapid growth, but still, these agents fail; why?
Major components of pancreatic cancer progression are pancreatic stellate cells, which play a major role in the metastasis and drug resistance of the cancerous cells.
Since the cancer cells may quickly become resistant to these chemotherapeutic agents, here is where technology comes into play.
Researchers at Purdue University have designed a unique microfluidic device that can be used to test a cancer drug on multiple tumor cell subtypes. With the help of this device, the management of cancer can be revolutionized as new drug therapies can be discovered, and existing medicines can be used more effectively.
Bumsoo Han, one of the Purdue leads on the research, said:
“The drug discovery and screening process has been using one cancer cell subtype and studying how it interacts with neighboring non-cancer cells, but this may overestimate the efficacy of the drug. By condensing time to look at how cancer cells interact within a pancreatic tumor, we found that one cancer cell subtype can not only be more drug-resistant than the others, but drug-sensitive cells can also become resistant through interaction between the subtypes.”
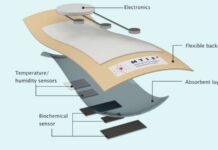
The microfluidic device gets its name from its intricately designed collagen channels that mimic the pancreatic duct on a very small scale. The microfluidic device provides a platform for the cancerous cells to proliferate and grow, and the mucro collagen channels can receive the drug therapies which are to be tested on the malignant cells.
Although there have been similar devices in the past, all of those could work on the late-stage malignant cells. Microfluidic device has been designed with a step-up unique ability to detect the drug response in the earlier cell lines that have not yet mutated. This may help to find out which therapies are most effective at preventing mutations from happening.