Antibiotics are one of the most powerful medications we currently have against diseases. Different antibiotics protect us from different bacterial infections. But what happens if these bacteria start to become resistant to antibiotic treatment? افضل طريقة للربح في الروليت
There are 3 levels of antibiotic treatment – subtherapeutic: when antibiotic concentration levels in the blood are too low to treat the infection; therapeutic: the perfect level at which the antibiotic can fight the disease; and toxic: concentration so high that it is dangerous for the body. العاب تجلب المال
Because treatment at subtherapeutic levels is not strong enough to affect the bacteria, the organisms get a chance to instead detect the threat and start mutating to a stronger, more resistant strain. Furthermore, the efficacy of the patient’s treatment also depends on maintaining optimum concentration levels.
To date, incorrect dosage has lead to countless antibiotic-resistant strains. In regular practice, doctors rely on previously determined pharmaceutical ranges which have usually been tested on animals or healthy populations. According to a new study published in Advanced Materials by researchers from the University of Freiburg, this type of “traditional TDM [Therapeutic Drug Monitoring] would be an extension of the “one-size-fits-all” approach, potentially resulting in subtherapeutic conditions and in turn, antibiotic resistance”.
New approach to Antibiotic Therapy
While a more individualized approach to determining optimal antibiotic dosage for each patient would be the most efficacious solution to this issue, the burden of continuous blood sampling would be difficult to incorporate in a clinical workflow. Therefore, scientists from the University of Freiburg have introduced a breath antibiotic biosensor. They call this a more “rapid, low-cost, sample-independent, and multiplexed on-site TDM” system in their article.
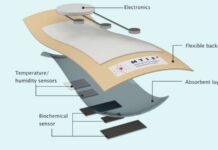
The microfluidic sensor carries bacterial proteins which react to beta-lactam antibiotics such as penicillin. Inside the sensor, enzyme coupled-beta lactam molecules are also present which compete with the antibiotic in the breath sample to bind with the bacterial proteins. This means that the more antibiotic is present in the breath, the less bacterial protein there is for the enzyme. العاب القمار على الانترنت The sensor is dependent on this enzyme’s product to indicate the presence of antibiotics in the sample.
According to the article, the researchers have tested their technology on pig models. They found that the biosensor showed a similar result to blood antibiotic concentration indicating that individualized testing may not require continuous blood sampling in the future.
One of the authors, Dr. Ceren Ates, explains that the technology may be incorporated in a conventional face mask. Meanwhile, the study’s corresponding author, Dr. Can Dincer, is working on another project to develop paper sensors that can continuously measure different biomarkers from the breath.
Source: The University of Frieburg