- Autoimmune keratitis includes a number of diseases with aetiologies derived from a dysfunctional immune system.
- It can cause an inflammatory destruction of the cornea.
- The clinical signs of autoimmune keratitis are often similar to those arising from infectious, allergic and neutrophic causes [1].
A 46-year-old woman presented to the ophthalmology clinic with complaints of blurring of vision, photophobia, tearing, redness and pain in both eyes. According to the patient’s history, the symptoms had been present since 7 days. On examination, the visual acuity of the patient in the right eye was 20/60 and in the left eye was 20/30.
The patient was started on treatment with atezolizumab, for metastatic bladder cancer two months earlier. Atezolizumab is an antineoplastic agent and antibody against PD-L1 (programmed dealth ligand 1) used for the treatment of hepatocellular carcinoma, small cell lung cancer, triple-negative breast cancer and urothelial carcinoma.
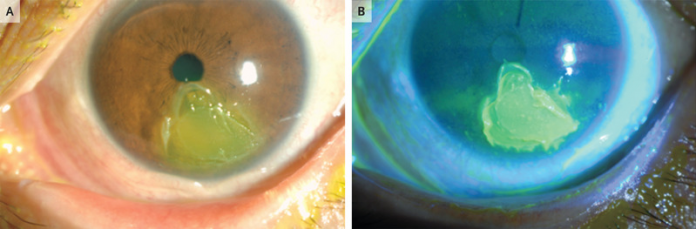
Further examination with a slit-lamp showed evidence of corneal epithelial damage (Panel A) in both eyes, pseudomembrane formation and conjunctival redness. In addition, fluorescein staining showed signs of overlying defect in the cornea with epithelial breakdown. In addition, corneal swab culture and polymerase-chain reaction assay was negative for herpes simplex virus.
The was suspected to have autoimmune keratitis and was started on treatment with topical prednisolone and atezolizumab was discontinued. One week after the treatment was initiated, the visual acuity of the patient improved to 20/20 in both eyes. Similarly, the corneal epithelium also showed signs of healing.
The patient was restarted on the prescription of Atezolizumab and continued to receive topical prednisolone. At 3-month follow up there were no signs of recurrence of keratitis [2].
References
- Gottsch, J. D. (2007). Autoimmune Keratitis. In Uveitis and Immunological Disorders (pp. 77-90). Springer, Berlin, Heidelberg.
- Oh, J. Y. (2020). Autoimmune Keratitis after Atezolizumab Treatment. New England Journal of Medicine, 383(15), 1468-1468.