This article describes the case of a 40 days old male infant diagnosed with Adams Oliver Syndrome.
The baby presented with cutaneous lesions and poor weight gain. Born through normal vaginal delivery at 38 weeks of gestation, he had a birth weight of 1700 grams. His Apgar score at 1 min of birth came out to be 8. It increased to 9 on a second evaluation after five minutes. There were no perinatal complications. The baby did not require any resuscitation or blood transfusion. However, the mother complained about poor feeding and vomiting during his neonatal period. He received only formula milk during this time.
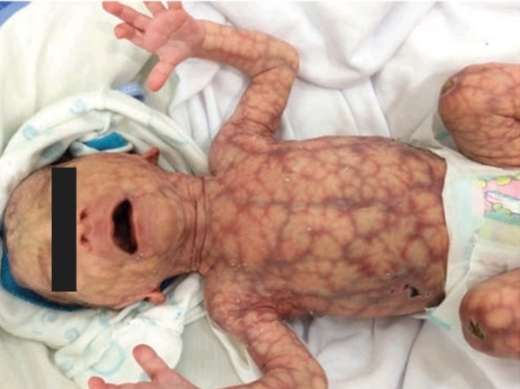
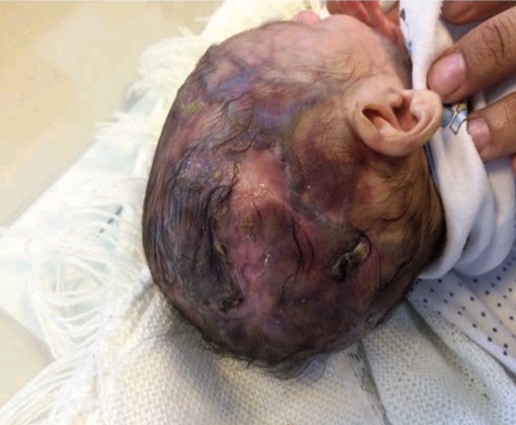
The child belonged to a healthy couple. The parents were cousins and he was their second child. The first one was also completely normal. However, this one showed a lot of abnormal features. He had a multiple vertex defect. Although his hands were normal, the patient’s feet showed signs of hypoplasia (in distal phalanges and nails). Moreover, skin examination showed generalized cutis marmorata along with dilated veins over the trunk and head. The infant also had glaucoma in the left eye.
The doctors performed some investigations to look for any coexisting visceral anomalies. An abdominal sonogram indicated a normal gut without any pyloric stenosis. The echocardiogram came out normal too. Doctors also ran liver and renal function tests and looked for serum electrolytes, all of which were normal.
Based on the scalp and limb defects and a consistently deteriorating body weight, doctors labeled the case as Adams Oliver Syndrome (AOS).
Adams Oliver Syndrome: An Insight
Adams oliver syndrome (AOS) is characterized by congenital scalp and limb defects which may be associated with multiple organ abnormalities. The scalp changes present as aplasia cutis congenita, a condition with agenesis of certain layers of the skin of the scalp giving it a thin transparent appearance. The primary limb defects are hypoplasia of distal phalanges and nails in the feet. Moreover, cutis marmorata (mottled and marbled skin) and poor weight gain also present quite frequently with the disease.
Adams oliver syndrome follows an autosomal dominant pattern of inheritance. However, it can also show autosomal recessive inheritance. Doctors have also observed sporadic cases of the disease, with or without a positive family history for AOS.
Pathogenesis
The exact pathogenesis of AOS is not known. However, various studies suggest impairment of vascular component as the main cause. According to several authors, organized thrombi in the placental vessels impair blood flow to the developing fetus which leads to impaired embryogenesis. Decreased perfusion to the developing structures leads to developmental anomalies which most commonly manifest in the scalp and the limbs.
Some authors propose that it is the small vessels that are corrupted with thromboembolic events gardening AOS. However, others suggest that interruption of blood supply from subclavian and vertebral arteries play the decisive role. Whatever the cause is, these vascular anomalies account for aplasia cutis congenita and limb defects seen in AOS.
Complications seen in Children with Adams Oliver Syndrome
Children with AOS have absence of scalp skin. This predisposes them to infections and bleeding. Moreover, these children display higher tendencies for raised intracranial pressures, seizures and cerebrospinal fluid leakage.
Moreover, they have fragile blood vessels. In about 20 percent of the cases, children bleed frequently. They are more vulnerable to bacterial infections than normal individuals. 23 percent of the cases show significant heart problems too. These include incomplete development of left ventricle (left ventricular hypoplasia), septal defects and pulmonary hypertension.
AOS takes a huge toll on the development of brain. Children with this syndrome often present with a small sized head, i.e., microcephaly. They often develop structural brain defects increasing their risk for epilepsy and seizures. Moreover, AOS affects their intellectual development as they have low IQ scores.
Less then 10 percent of the cases develop eye problems too, including cataract, strabismus and optic nerve atrophy.
Diagnosis of AOS and Related Disorders
Many other conditions present with somewhat similar features as AOS. Skin-ear-nipple syndrome involves scalp malformations (hairless skin) and underdeveloped ears and nipples. Cutis marmorata talengectasia congenita manifests in the form if patches of discoloured skin that are similar to the ones in AOS. Similarly, poland syndrome involves short webbed fingers that can be confused with limb defects seen in AOS. Thus for diagnosis of AOS, doctors look for both scalp and limb defects. Moreover, they confirm it through genomic studies which reveal mutations in autosomal genes. Diagnosis can also be made if the patient has only one of the two presenting features but is positive for specific AOS mutations.
Treatment
Treatment of AOS involves a multidisciplinary approach. It brings together paediatricians, orthopaedic surgeons, plastic surgeons, cardiologists and ophthalmologists. All of them provide symptomatic and supportive care to the patient. In general, scalp defects heal without treatment. However, extensive malformations may require surgical grafts. For limb defects, doctors usually employ physiotherapy or the use of artificial limbs. The patients are strictly monitored for any cardiac malfunctions. They also undergo regular ophthalmological assessments to look for any eye problems that are seen in such patients.
The patient did not have any associated organ system defects. His major complaints were vomiting and weight loss apart from scalp and limb manifestations of the disease. Doctors substituted regular formula with hydrolyzed formula as a treatment for predominant symptoms. The vomiting improved. However, poor weight gain did not resolve. The infant reached a weight of only 2200 grams at 2 months of age.