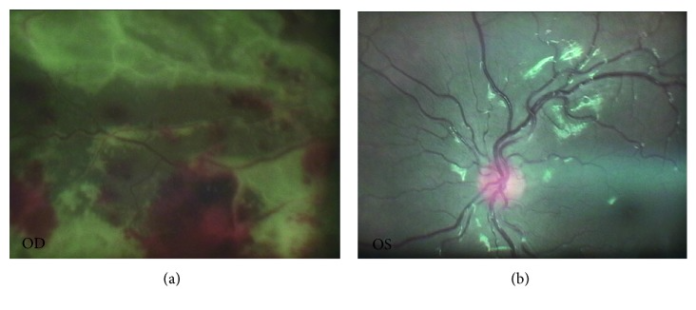
Acute progressive visual loss due to cytomegalovirus in 12-year-old with acute myeloid leukemia.
This article describes the case of a 12-year-old boy who presented with acute progressive visual loss and acute myeloid leukemia (AML). The patient was admitted to the hospital for febrile neutropenia after his last course of chemotherapy. He was given the FLAI regimen, including fludarabine, cytarabine, and idarubicin. Doctors started him on cotrimoxazole with prophylaxis dosage after a full sepsis workup.
The patient was also prescribed voriconazole because of his previous history of pulmonary aspergillosis as fungal prophylaxis. Doctors advised a blood culture which was positive for viridans streptococcus. The patient developed high-grade fever on 48 hours after admission. In addition, he developed acute vision loss on the 6th day of admission, despite being prescribed antibiotics. However, the patient’s neurological exam was normal. Doctors suspected the patient of having retinal detachment and cancer associated with retinopathy. Variconazole was replaced with lipsomal amphotericin B. The blood samples were sent for a new culture because the high-grade fever did not resolve on even on the 8th day of therapy. Similarly, a chest X-ray was also done. However, with no significant findings.
Toxoplasmosis IgM levels were negative, including other fungal and viral pathologies.
Another X-ray was requested on the 10th day of admission because of the patient’s poor condition. However, there were no significant findings on the chest X-ray. Doctors further added Rifampin and linezolid to the patient’s regimen. Although, the linezloid was replaced with vancomycin on the 12th day of admission because of persistent bacteremia.
The patient also complained of deteriorating visual function in the right eye. He was referred to an ophthalmologist on the 16th day of admission. Examination was significant for fluffy lesions with diffuse retinal hemorrhage and patchy focal necrosis in the right eye. The right eye was normal. Doctors performed a vitreous aspiration under general anaesthesia, with suspicion of cytomegalovirus (CMV). Further investigations confirmed the presence of CMV. He was therefore given injections of ganciclovir 1 week apart with adjunctive systemic antiviral therapy with ganciclovir on the 24th day of admission.
The plan was to continue the treatment for 4 weeks. However, unfortunately, the patient died because of poor response to chemotherapy 8 weeks after admission.
References
Acute Progressive Visual Loss in a Case of Acute Myeloid Leukemia: Challenges in the Utility of Molecular Tests in Early Diagnose of Cytomegalovirus Retinitis https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5831968/