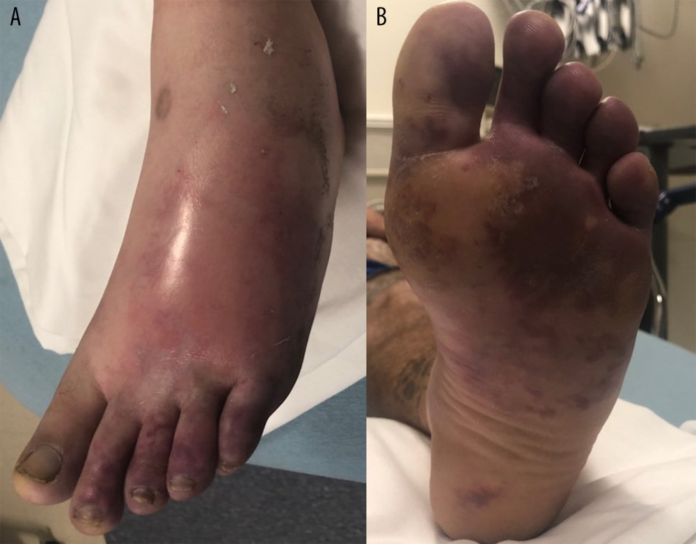
Case study: acute limb ischemia
This article describes the case of a 35-year-old man who presented to the emergency department with opioid use disorder (OUD) complicated by multiple SSTIs. He would inject heroin into his bilateral feet, forearms and groin. His history also revealed that although he got the needles from a syringe service program, he would often lick and reuse the needles. In addition, he also revealed sharing the injection equipment, including needles with monogamous sexual partners. This raised suspicion for infectious complications of IDU. However, further evaluation findings were consistent with the diagnosis of acute limb ischemia.
On examination, the patient’s dorsal surface of the foot was erythematous, swollen and tender. In addition, although not warm, it had a patchy dusky purple discolouration. The patient described the pain as severe, burning and non-radiating. The examination further showed full strength and sensation in the entire limb with reduced motor activity in the great toe and tenderness throughout the foot. Doctors further advised laboratory tests that showed an elevated creatinine kinase (CK). Whereas urine toxicology was positive for cannabinoids, fentanyl, oxycodone/oxymorphone, and opiates. The fentanyl was most likely present in the urine because of illicitly manufactured fentanyl. And the oxycodone because of the oxycodone he received in the emergency department prior to providing the specimen. Similarly, the opiates were most likely because of morphine.
The diagnosis was still unclear at this point
The differential diagnoses for his presentation included necrotising fascitis, SSTI with or without abscess and compartment syndrome. Given the patient’s history of SSTIs and his physical presentation, doctors diagnosed him with skin and soft tissue infection. Doctors started him on empiric vancomycin. Orthopaedic and soft-tissue surgeons further evaluated the patient and suspected him of having a necrotising soft-tissue infection. Doctors immediately shifted him to the operation room. However, surgical findings ruled out necrotising SSTI and compartment syndrome.
Given the patient’s SSTIs history and elevated inflammatory markers, the patient was diagnosed with skin and soft-tissue infection. Doctors started the patient on empiric vancomycin. Orthopaedic and soft-tissue surgeons suspected necrotising soft-tissue fascitis. He underwent a successful closure of the surgical wound, however, continued to report severe pain.
On further questioning, the patient revealed that he made several unsuccessful attempts for locating a site with good blood return before he injected it into his left foot. Similarly, a small amount of blood had collected in the syringe and clotted. He injected the contents of the syringe including both the drugs and a small thrombus. Thinking that it was a vein on top of his left foot. He was surprised to learn that he had injected himself into an artery. He could not tell the difference, nor did he know that the distinction was important. His medical history and presentation led to the diagnosis of acute limb ischemia.
Treatment
Doctors treated him with intravenous heparin and referred him for a vascular surgery consultation. He was further referred for opioid replacement therapy and a multimodal treatment plan including, aggressive hyperbaric oxygen therapy and therapeutic anticoagulation.
Source: American Journal of Case Reports



