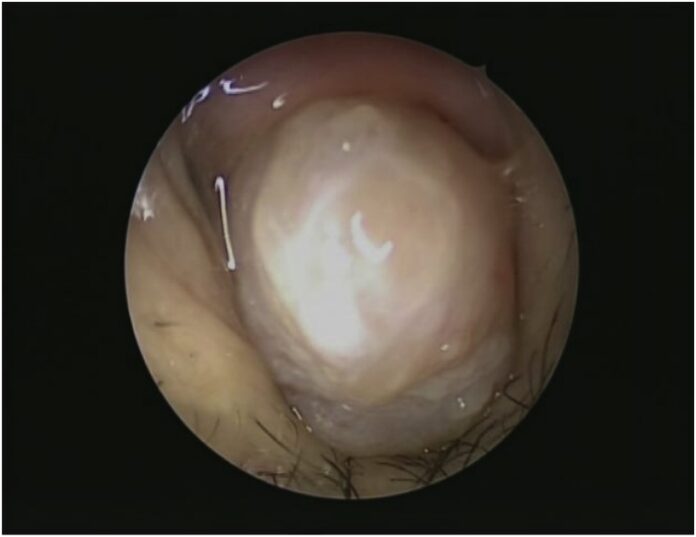
Case Presentation
A 64-year-old Saudi female presented a several-month history of recurrent episodes of epistaxis and unilateral progressive nasal blockage. Anosmia, nasal discharge, congestion, sneezing, face pain, or headaches were not previously reported. She had previously been diagnosed with diabetes and hypertension. Other than that, her family history was unremarkable.
A rigid endoscopic examination of the nose revealed a significant left-sided polypoidal tumour with smooth overlaying mucosa. Furthermore, it completely blocked the left nasal canal. There was no palpable lymphadenopathy, and the entire ear, nose, throat, head, and neck examinations were all normal.
Investigation
A CT scan of paranasal sinuses was done with contrast, which revealed a left anterior lobulated nasal mass at the level of the cartilaginous section of the nasal septum, along with modest heterogeneous post-IV contrast enhancement and bone remodeling. There was no extension to the paranasal sinuses, and no apparent bone invasion was seen.
Endoscopic Procedure
Endonasal endoscopic excision of the left nasal cavity was carried out under general anaesthesia. Intraoperative examinations revealed a semifirm vascular mass attached to the anterior aspect of the middle turbinate and septum at the same level. The pedicle was cauterized after the mass was fully removed from its attachment. Three fragments of soft to firm tan-grey tissue, the largest measuring 1.8 x 1.6 x 0.6 cm and the smallest measuring 0.8 x 0.6 x 0.5 cm, were found during a histological investigation of the mass.
The lesion was positive for vimentin and S100 and negative for desmin, NSE, and SMA.
The final histology supported the diagnosis of nasal septum schwannoma.
Apart from that the patient has had frequent follow-up care for three years with no recurrence.
Discussion
Nasal septal schwannoma is a rare finding, with only 32 reported cases in the literature.
It is commonly observed in adults in their late 40s and 60s with no sex predilection.
Nasal septal schwannoma commonly affects the posterior aspect of the septum and is thought to develop from the trigeminal nerve’s nasopalatine branch. Nasal blockage, anosmia, distortion of the nasal pyramid, headache, and epistaxis are typical symptoms.
The results of a CT scan do not always indicate the presence of schwannoma. However, CT is useful in determining the location and size of the tumour. MRI is preferred over CT for separating tumours from inflammatory conditions and normal tissue, and it also offers information on the tumour’s intracranial invasion.
However, the diagnosis of nasal septal schwannoma is mostly dependent on biopsy or complete excision of the mass because imaging is non-specific for schwannoma.
Schwannomas can be seen macroscopically as well-defined, enclosed cystic masses that are attached to the nerve tissue. Schwannomas can be divided into Antoni A and Antoni B patterns based on their microscopic characteristics. Spindle cells arranged as cellular regions with nuclear palisading make up Antoni A patterns while myxoid stroma that is loose and disorganized with few spindle cells characterizes Antoni B patterns.
The ideal treatment for nasal septal schwannoma is the surgical removal of the mass, which can be accomplished with either lateral rhinotomy or endoscopic endonasal surgery. The common surgical technique for removing tumours is the endoscopic endonasal approach with or without imaging guidance