A 54-year-old male succumbed to death secondary to an intracranial haemorrhage which was most likely due to sildenafil use for treating erectile dysfunction.
A wife brought her 54-year-old husband to the emergency department after he lost consciousness. The wife, while explaining the preceding event, told that around 4 hours earlier, her husband suddenly started complaining of dizziness, nausea, and vomiting while chatting with her. Thereafter, he got confused and couldn’t comprehend what others were saying. Finally, he fell unconscious. She also revealed that lately, the patient was having problems with an erection so his urologist had prescribed him sildenafil for erectile dysfunction. He, for the first time, had taken 2 tablets of sildenafil (100 mg) approximately 3 hours before the symptoms began, to attempt sexual intercourse.
Past medical history revealed no use of sildenafil, diabetes, hypo- or hypertension, and hyperlipidemia. The patient had been otherwise healthy and normotensive. He did not use any regular medications. Moreover, he didn’t smoke or used illicit drugs. Additionally, he had no family history of cerebral arteriovenous malformation, cerebral aneurysm, or intracranial haemorrhage.
Examination:
On examination, his blood pressure was 130/85, heart rate was 104 beats per minute, and his body temperature was 37.1 C. He was confused and disoriented. Neurological examination revealed an extension response to pain and he was making incomprehensible sounds. The Glasgow Coma Score was 6. He had small (1.5 mm) pupils bilaterally with absent direct and indirect pupillary light reflexes. However, there was no eye deviation. Motor examination revealed no asymmetry in muscle strength and tone. Reflexes were 2+ and symmetric in upper and lower extremities bilaterally. Bilateral plantar reflexes were absent.
Auscultation of the chest revealed bilaterally rough breath sounds.
Serological investigations were unremarkable with normal platelets and coagulation profile. Urine toxicology was also unremarkable.
In the emergency department, the patient developed respiratory distress, therefore, the doctors intubated him. Thereafter, they shifted him to the neurology intensive care unit (ICU).
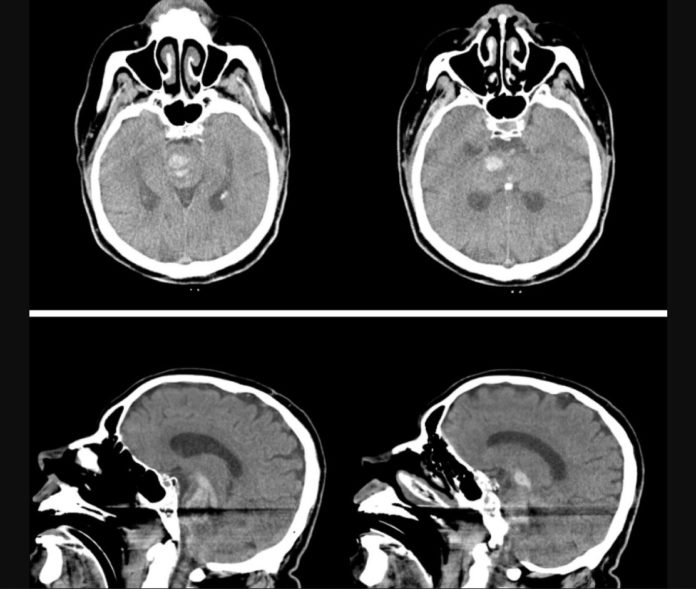
Cranial computed tomography (CT) scan revealed a hyperdense area (hematoma) with vasogenic oedema. The doctors suspected that the hematoma had started from basal ganglia level and spread to mesencephalon and pons, inferior and to the 4th ventricle and pontocerebellar level in the posterior. However, the CT scan did not reveal any vascular anomaly or any other evidence to suggest the cause of intracranial haemorrhage.
The doctors made a working diagnosis of intracranial haemorrhage secondary to sildenafil use after excluding other aetiologies of ICH.
The patient received mannitol to counteract oedema.
Unfortunately, on the 5th day of hospitalization, he developed acute renal failure so he stopped receiving mannitol after a nephrology consultation. He underwent dialysis.
On the 12th day of his hospital stay, he succumbed to death despite adequate treatment and inotropic support.
The relatives denied autopsy.
Sildenafil citrate is a potent vasodilator which is prescribed for treating erectile dysfunction. ICH is a rare but fatal complication of sildenafil. Other common side effects include headaches, flushing, nasal congestion, dyspepsia, respiratory infection, dizziness, and visual disturbances. However, among the side effects, ICH remains the most fatal adverse effect as the mortality rate is 40% in the first 30 days.
During sexual activity, the cerebral blood flow increase. Concurrent use of sildenafil can further increase the flow to the brain as a result of its vasodilating effect. Consequently, the risk of haemorrhage increases. bwin
It is imperative to educate the patient and discuss the risks vs. benefits of sildenafil before prescribing it. Moreover, when prescribing, it is crucial to start with the lowest dose to ensure safety. ترتيب البوكر
Reference:
Murat G, Hakan C, Fatma G, Goncagul T, Unal B, et al. (2020) Intracranial Hemorrhage Associated with Sildenafil Use: A Very Rare Complication. لعبه بلاك جاك Int J Neurol Neurother 7:099. doi.org/10.23937/2378-3001/1410099