- Multiple sclerosis is commonly describes as a disease of young Caucasian females.
- While the prevalence is higher in Caucasian females, the real incidence is actually higher in African Americans.
- This case highlights the implications of MS in an older African American male.
This article describes the case of a 53-year-old African American ex railroad worker with a 4.5 year history of multiple sclerosis implications. The patient presented with complaints of back pain and weakness in the right arm and bilateral lower extremity and spasticity. The weakness and spasticity were acutely worsening which disabled him from moving from his bed to his rolling walker.
Medical history
His medical history revealed an open reduction internal fixation of the left ankle because of a motor vehicle accident. In addition, his history further revealed cocaine and heroin use and daily use of methadone. He also complained of chronic back pain with the motor vehicle accident as a contributing factor. He was admitted to the hospital multiple times since March 2014. The patient was 48 years old when he was first admitted for back and leg pain with lower extremity weakness. Doctors advised imaging at the time which showed foraminal stenosis, anthropathy and multilevel disc herniation in the cervical and lumbar regions.
He further reported that he was self-medicating with oxycodone and sniffed heroine to alleviate the pain and muscle stiffness. This also helped him walk better. Doctors would always discharge him on naproxen with follow-up advise as an outpatient with a neurologist. However, he was unable to report to any of the follow-ups because of a loss of driving capability and lack of conveyance. His weakness reached a point where he needed a rolling walker for support. He described the pain as sharp and stabbing on each presentation. In addition, he also complained of intermittent numbness and tingling with the pain.
Family history was only significant for hypertension. Whereas his social history revealed that he used 30 packs of in a year. He occasionally consumed alcohol. There was no history of allergies and his systems review was negative for changes in appetite, eye pain, weight loss, chills, fever, urinary and bowel changes.
Physical examination
Physical examination showed hypertonicity of the muscles, bilaterally in the thighs, calves and ankles. His patellar and Achilles reflexes were 3+ bilaterally, whereas 3+ in the right brachioradialis and triceps. Examination further showed a “swinging gait”. The rest of the examination was unremarkable. His lab work was also unremarkable except for anaemia with low hemoglobin.
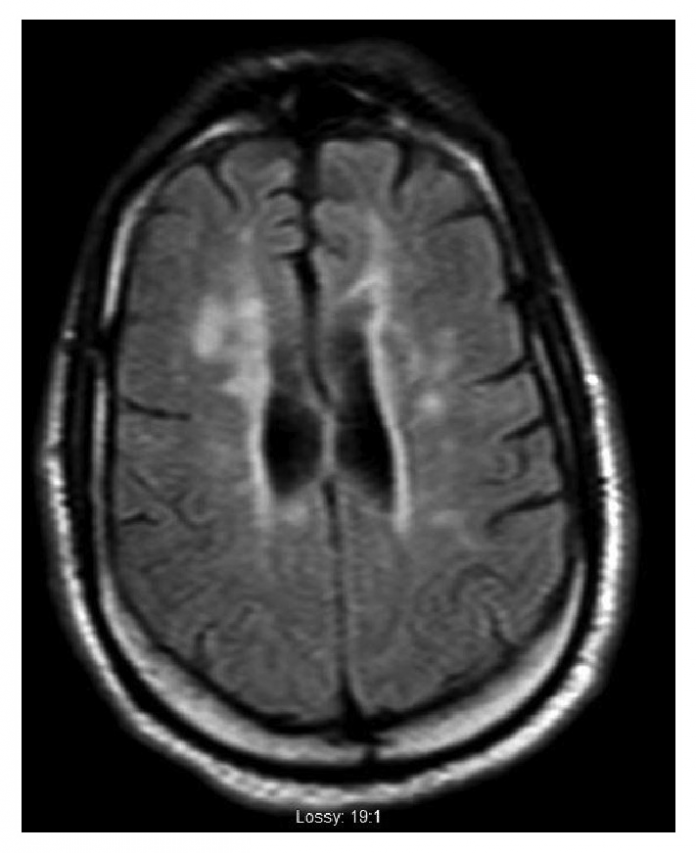
Lumbar CT showed similar findings as the previous CT scan. However, a new T2 hyperintense lesion was noted at the conus medullaris, measuring 1 cm at the level of T12/L1. The finding suggested a demyelinating disease. MRI of the cervical spine also showed abnormal T2 FLAIR enhancement from C2 to C6. Although, no optic involvement was evident. Lumbar puncture did not show any evidence of an infection either.
Doctors diagnosed the patient with multiple sclerosis using the McDonald criteria based on imaging findings and clinical presentation. Treatment included methylprednisolone which improved symptoms drastically.
References
Unmasking the Masquerader: A Delayed Diagnosis of MS and Its 4.5 Years of Implications in an Older African American Male https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6702817/